Why ABT Tests Cortisol in All Female Athlete Panels
ABT SheConquers Series
Training is a repetitive cycle of stress and recovery. When balanced, the cycle leads to cumulative performance gains. But, if the scale tilts too heavily to stress or recovery, optimal performance gains are impossible. Prolonged excessive stress puts athletes at risk of a condition known as overtraining or overreaching syndrome. This condition devastates performance and turns daily exercise into a chore rather than a pleasure. Performance deficits can be short-term or long-term.
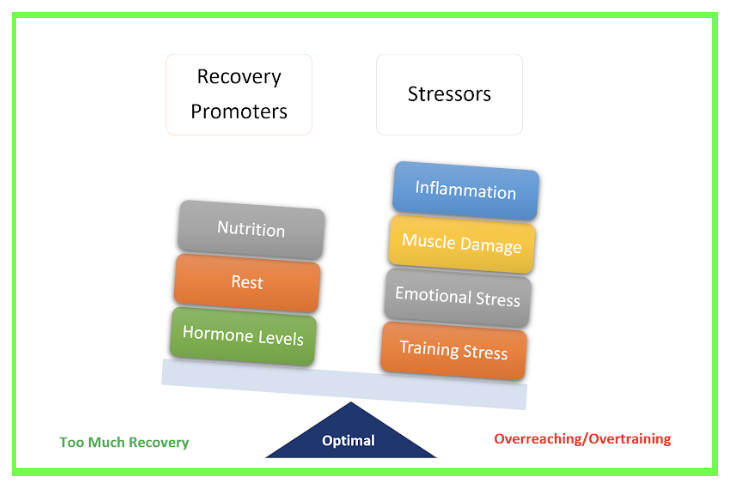
There is no one-size-fits-all to maintaining the balance of the stress-recovery cycle. Female athletes are more prone to overtraining syndrome. Proneness also varies by individual. Individuals vary in their ability to recover from muscle damage, hormone fluctuations associated with exercise, and inflammatory response.

| Ideal Training Cycle | Dietary Influences | Other Recovery Liabilities | |
| Athlete A | 4 Endurance Days, 2 HIIT Days, 1 Recovery Day | Low Genetic Affinity for B12 and Folate | High-Stress Career, Mother of 2, Heavy Periods, low free testosterone, oral contraceptive |
| Athlete B | 3 HIIT Days, 2 Endurance Days, 2 Recovery Days | High Iron AbsorptionLow Folate Absorption | Difficulty controlling diet due to career as a sales rep, training in early mornings or evenings, high cortisol |
| Athlete C | 1 HIIT Day, 5 Endurance Days, 1 Recovery Day | GI inflammation reduces the absorption of iron and folate | Vegetarian, celiac, oral contraceptive, high inflammation following training sessions |
A critical blood test used to screen stress-recovery balance is cortisol.
Cortisol is a hormone secreted from the adrenal glands (above your kidneys). Cortisol is involved in many physiological processes critical to athlete performance, including:
- Fat metabolism (fat storage and energy)
- carbohydrate metabolism (energy)
- Inflammation control (recovery)
- Stress response (performance and recovery)
- Electrolyte regulation (performance)
- Protein metabolism (performance)
Cortisol, commonly referred to as the “stress hormone,” elevates in response to physical and psychological stress. Rapid elevations in cortisol are associated with hypervigilance, an enhanced state of sensory sensitivity accompanied by an exaggerated intensity of behaviors whose purpose is to detect activity. You know those moments when you are focused, responsive, and “on your game”? Cortisol is involved in this state of awareness.
Although cortisol is useful in game-time situations, chronically high or low levels indicate an unbalanced stress and recovery cycle. Most often, if stress (physical and/or psychological) is heightened for a short period of time (days to weeks), cortisol levels will be elevated. If stress is heightened for an extended period of time (months), cortisol levels can become chronically low.
In chronic stress states, elevated or low cortisol can lead to weight gain, sleep disorders, tissue breakdown (tendonitis), uncontrolled inflammation, suppressed immunity, and interference with other vital hormones (such as the proper function of the thyroid hormone). This condition is pretty rare among ABT users. However, slipping into a temporary state of prolonged high cortisol is not uncommon. ABT users commonly report faster time to fatigue while training, prolonged recovery from workouts, food cravings (especially sugars), and elevated heart rate while training when this occurs.
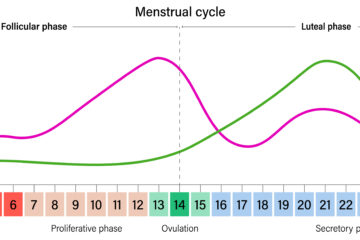
Cortisol is especially important for female athletes to balance because of its association with the hormone progesterone and oral contraceptives. Progesterone levels influence the cortisol response. Women have higher progesterone levels than men, and levels vary depending on the stage of the menstrual cycle. The combination of elevated cortisol and progesterone levels in female athletes makes it crucial for women to focus on proper recovery to lower cortisol levels post-workout. Additionally, oral contraceptives may also impact the cortisol levels in female athletes by causing an increase in total and free cortisol.
Pro runner Rebecca Mehra, of the Oiselle Littlewing Running Team, monitors cortisol as part of her regular Athlete Blood Test. ABT asked Rebecca to explain how she integrates blood testing into her training.

“
Rebecca shares,
Until the past year, I did not regularly have my blood tested for performance purposes. Making that change has been a huge key to staying healthy while training.”
I had three major findings in my first series of blood tests:
1) Low folate
2) High cortisol
3) Low vitamin D
All three of these findings led me to make changes in my lifestyle and diet for the better, as I followed the ABT Sports Scientist’s suggestions. I started to cook and eat more cruciferous vegetables on a daily basis. I put in more effort to take naps and sleep an extra hour per night in hopes of bringing my cortisol down. I started supplementing vitamin D with the recommended brand.
Over the next several months and subsequent tests, all of these findings normalized, thanks to the ABT suggestions that I followed meticulously! Getting my blood tested and following the ABT suggestions is now one of the more important tools in my training arsenal.”
Margo’s Take on Cortisol

Elite runner and Nutrition Therapy Practitioner Margo Malone of ABT discusses some of the strategies she uses to help keep cortisol in check.
Focus on four key elements: nutrition, sleep, stress management, and recovery.
- Nutrition:
- I Aim to begin my recovery process within the first 30 minutes after a hard effort to start repairing the muscle and get the cortisol as low as possible.
- 25-30g of really good, high-quality protein, with 50-60g of carbohydrate to facilitate that protein uptake.
- Why? Without proper nutrition, the body will recognize a starvation state as an additional stressor and further elevate cortisol levels to help mobilize stored fats and sugar from the liver. Not eating after a big workout and getting too few calories in your day sends a stress message to your hypothalamus and can result in cortisol secretion. It is crucial to maintain healthy blood sugar levels with proper macronutrients (carbohydrates, proteins, and fats) to stimulate recovery. When blood sugar levels are too low, cortisol is released to increase the fuel available to the heart and skeletal muscles (Stachowicz & Lebiedzinska 2016).
- Pro tip: Try adding a little protein, such as yogurt, before bed to help stabilize blood sugar during sleep to keep cortisol down
2. Sleep:
- I try to keep consistency in sleep schedules and get at least eight hours a night.
- Why? Sleep is a crucial part of recovery. Unfortunately, elevated cortisol may be a primary cause of sleep disorders (Schatzberg 2005). Our body uses sleep to restore homeostasis and repair.
- Pro tip: Develop a routine each night to help your body prepare for bed. Try a cup of chamomile tea and light stretching to wind down.
3. Reduce Life Stress:
- I recommend methods such as yoga, deep breathing, reading, cooking, and connecting with friends.
- Why? Just like physical stress, emotional stress can also play a role in elevated cortisol levels.
- Pro tip: Take time to identify significant stressors in everyday life and prioritize activities your find to relieve stress.
4. Recovery Days: The training model of stress/recovery only works appropriately if both sides are treated equally. Take your recovery days as seriously as your workout days. After all, lowering cortisol levels after workouts is just as crucial to future performance as hitting your workout splits!
Sources:
Stachowicz, M. & Lebiedzińska, A. (2016). The effect of diet components on the level of cor(sol. European Food Research & Technology. 242: 2001.hlps://doi.org/10.1007/s00217-016-2772-3
Buckley T, Schatzberg Z. On the interactions of the hypothalamic-pituitary-adrenal (HPA) axis and sleep: normal HPA axis activity and circadian rhythm, exemplary sleep disorders. J Clin Endocrinol Metab. 2005; 90(5):3106-3114.
Front Integr Neurosci. 2012; 6: 66. Published online 2012 Aug 28. doi: 10.3389/fnint.2012.00066PMID: 22973203Time-dependent effects of cortisol on selective attention and emotional interference: a functional MRI study. Marloes J. A. G. Henckens,1,2,* Guido A. van Wingen,1,3 Marian Joëls,2 and Guillén Fernández1,4